At a meeting with National MP Erica Stanford during strike action recently, we raised concerns about patient safety and staffing shortage.
Stanford was the only Government MP willing to meet with us. About 20 of us packed into her Auckland East Coast Bays’ office to warn her that tight budgets were driving substandard care — including the use of incontinence pads to dress ulcerated legs.
We told her we held grave fears for our patients.
Waitematā’s district nursing dervice operates from North Shore and Waitākere to the Hibiscus Coast, Helensville and Warkworth. Our service is designed to prevent avoidable hospital admissions, support early discharge, and promote patient independence.
However, staffing shortages are seriously undermining that goal.
How dire is the situation when, in 2026, nurses in Aotearoa are resorting to incontinence pads to treat ulcerated legs?
“We’re given so many patients each morning that I have to decide who will be seen today and who won’t,” one nurse said in the hui.
Along with the struggle to provide safe wound care, we told her that severely limited staffing was also forcing us to make difficult decisions about who to treat and who to defer.

We explained that these are not small wounds. There are ulcerated legs — some patients even have them on both legs.
We are trying to manage higher and more complex case loads, with limited time. This forces us to make difficult decisions that affect Kiwis’ lives.
We also highlighted the social impact of missed visits, noting that for some patients, district nurses provide their only regular human contact. Repeated deferrals left patients frustrated. At times, they directed their anger at frontline staff. Nurses reported experiencing verbal abuse as a result.
We told her that when patients were not seen promptly, their condition often deteriorated, requiring more intensive treatment and extending time in the service or requiring hospital care.
One of the most confronting examples we shared is the use of incontinence pads to dress leg ulcers, which is far from best practice. This is both humiliating for patients and deeply frustrating for us.
Inadequate funding ‘punishing’
With the current budget pressures and workforce shortages, we questioned whether funding has kept pace with rising demand given population growth, an ageing demographic, increased administrative requirements and higher costs for wound care supplies.
“It feels like a direct punishment,” one nurse said at the meeting, of the budgetary constraints.
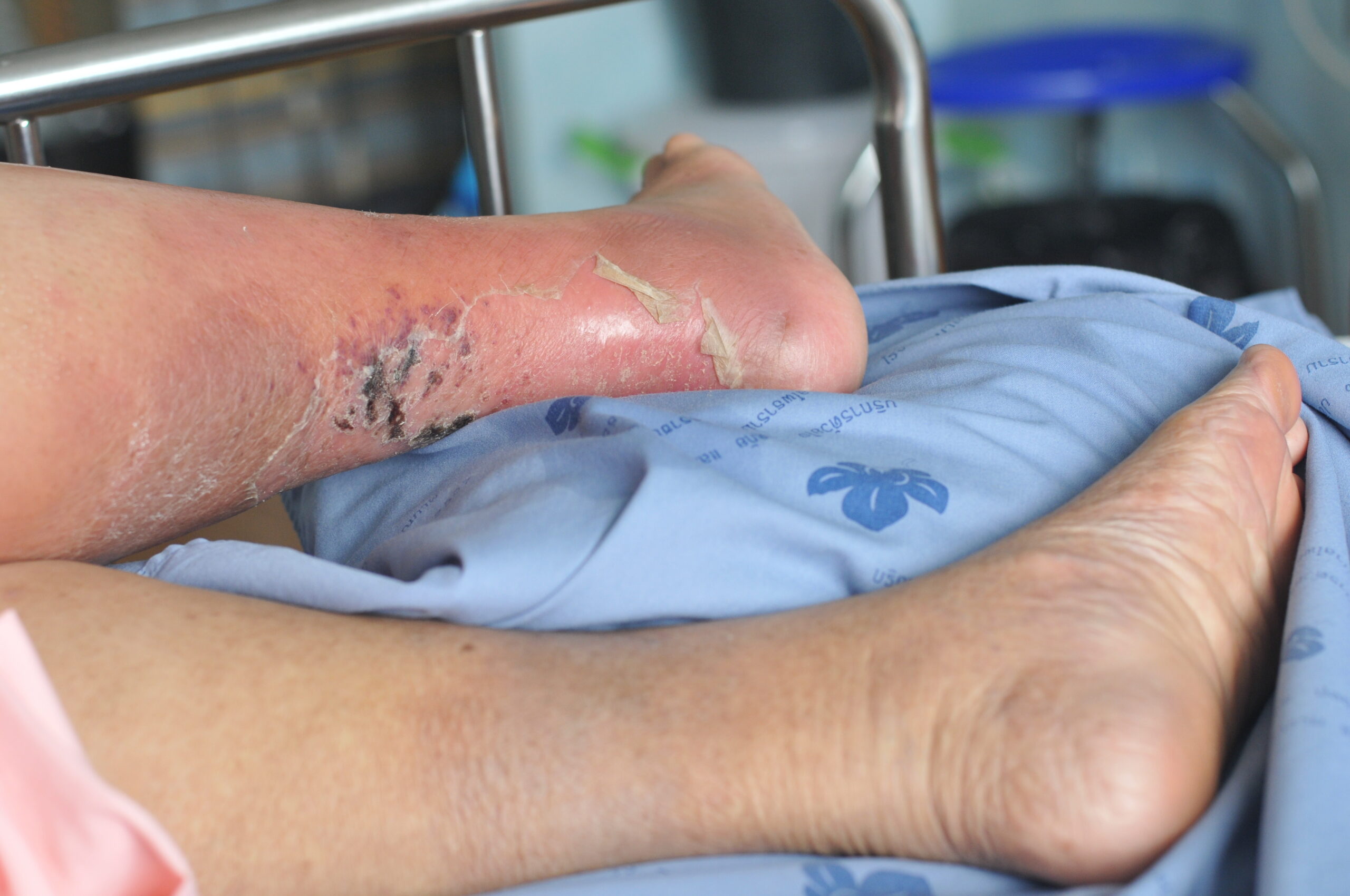
How dire is the situation when, in 2026, nurses in Aotearoa are resorting to incontinence pads to treat ulcerated legs?
Stanford acknowledged and voiced her understanding that delays in care can lead to hospital admissions and poorer long-term outcomes.
For some patients, district nurses provide their only regular human contact.
However, as district nursing did not fall within her ministerial portfolio, she said she could not comment directly. However, she agreed to raise the nurses’ concerns with Minister of Health Simeon Brown — noting that a system review was already underway.
“Will he listen to you, though?” we asked.
“He is a pragmatic guy,” Stanford replied.
And you know what, pragmatism is exactly what is needed now!
But a pragmatic approach means dealing with these problems realistically, with a focus on practical outcomes.

In wound care, the consequences of delayed treatment are clear: wounds worsen, require more intensive care, demand more staff time, consume more resources, and ultimately increase hospital admissions. In some cases, the consequences can be life-threatening.
The solution, we believe is equally clear: adequate staffing to ensure timely, effective care at the first point of contact.
We fear the current review of the service is trying to turn health care into a money-driven business.
How do we bring it back to a care-based approach?
–Roseanne Maber is a district nurse based in Waitākere. Michelle Beard is a freelance photojournalist.
The nurses also visited Labour’s Te Atatū MP Phil Twyford; Green Mt Albert MP Ricardo Menéndez March and Labour’s Auckland spokesperson Shanan Halbert. Labour’s North Shore candidate Sam Collins also attended.
Both ministers respond
Auckland East Coast Bays’ MP Erica Stanford — also Minister of Education and Immigration — said she would be passing on her local district nurses’ concerns to the Minister of Health Simeon Brown.
Brown told Kaitiaki district nurse staffing shortages were a matter for Te Whatu Ora-Health NZ (HNZ). However, he “greatly values the work of our district nurses and appreciates everything they do for their patients and communities”, a spokesperson said.
National chief nurse Nadine Gray has said the district nursing service is being reviewed nationally to assure safe staffing across HNZ. No time frame has been provided.




