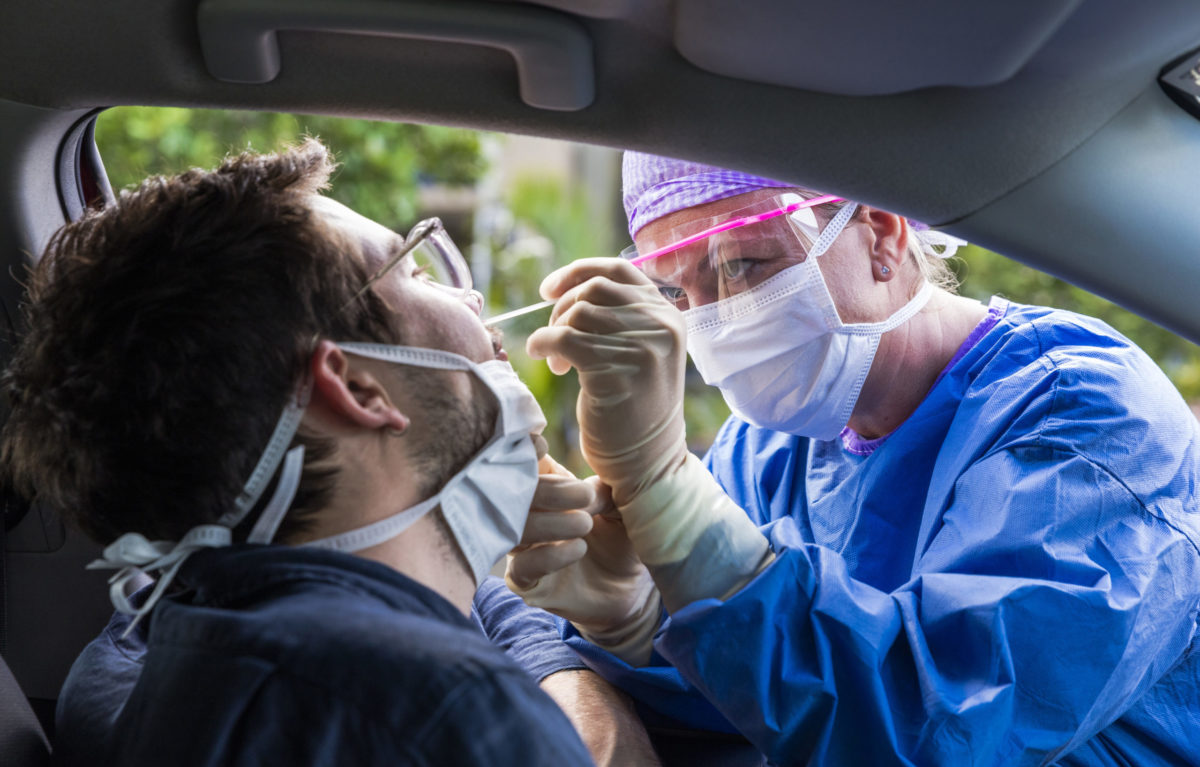
People are experiencing extraordinary challenges under the COVID-19 pandemic. It is affecting the wellbeing of individuals and those around them, and the livelihoods of people and communities. It also has a major impact on the public who find themselves (quite literally) at the sharp end of testing and vaccination efforts.
As health practitioners, we need to understand that what might seem like relatively minor issues for us can be barriers to testing and vaccination for the population in general. Decisions we make about practical issues such as the type of testing and injection technique matter; the language we use to talk about these things, and the images we use, all convey messages. Reflecting on these things and changing how we act and what we say has the potential to help testing and vaccination efforts.
The position of health professionals
Most of us have not lived through a pandemic before, but those familiar with the world of health professional practice have a head-start in understanding what has unfolded across the world in the last 18 months. We understand that clothing normally used in hospital and laboratory settings is now being worn in the community. It is likely that we knew that PPE is the abbreviation for “personal protective equipment”, ie masks, face shields and gowns.
We can probably navigate our way through an article in the media that includes many references to percentages, when summarising the vaccination rates. It is also likely that we could figure out how an mRNA vaccine differs from others we have come across, and relevant details of “the science”.
We probably also appreciate the need for testing and vaccination, but it is critical to reflect on how the public see, experience and understand these two procedures. When people are being exhorted to get tested or vaccinated, we need to think about the role we might play in overcoming any barriers they experience.
There are many barriers and it is likely that the institutional, cultural and geographical ones are among the greatest. Genuine access is key to equality and if we ever needed reminding of the importance of understanding where people are, what matters to them, and how to engage with them, then this is the moment. Health-care staff can improve access through building relationships and rapport with people.1
On a daily basis, many of us perform tasks that that are invasive, and risk inflicting pain and discomfort on others.
Health professionals have a practical understanding of testing and vaccination. On a daily basis, many of us perform tasks that that are invasive, and risk inflicting pain and discomfort on others. The challenges health professionals face as they work in risky settings, manage uncertainty, and interact with people experiencing stress are recognised as problematic in specific settings2 and also in the context of the COVID-19 response.3
A practitioner may pay minimal attention to inflicting pain and discomfort, or minimise it as only being for a few seconds for each patient, as a useful strategy in a crisis, enabling them to keep going. But it is likely that long-term this could have a detrimental impact on the practitioner’s wellbeing.
The fact that home-based screening for cervical cancer in Aotearoa New Zealand has only recently been introduced is an example of our slowness to adopt less-invasive approaches to screening, which has had a significant impact on access for Māori women.4 The cervical screening issue is another reminder to think about equality in terms of access, culture, and context.
Invasive language
Using the terms “shot” or “jab” to refer to a vaccination presents the procedure as violent. While this is not a problem for many people, this kind of negative context could be a barrier for some. The concept of a “shot” could be offensive and provocative for people who come from cultural backgrounds in which gun violence is a problem. This is exacerbated when asking people if they have “been shot”.5 The term “jab” can sound equally violent. It also involves one person performing this act upon another, which links a power dynamic (necessary when giving vaccinations) with violence.
It is common in health care for metaphors to have negative connotations. The concept of a “battle” or a “war” is often appropriated in relation to cancer treatment.6 We need to consider the consequences this language may have for people. Even if this is only an issue for a very small group, it is reasonable to suppose that they will be among those reluctant to be vaccinated.
Using the terms ‘shot’ or ‘jab’ to refer to a vaccination presents the procedure as violent. While this is not a problem for many people, this kind of negative context could be a barrier for some.
We know that language matters and, in the context of COVID-19, Aotearoa New Zealand has done well to convey a generous and supportive approach,7,8 including reference to the “team of five million”.
However, talking about people who have tested positive as “cases” has the tendency to define them as curiosities and other than human. People with the virus are just that – “people” who have the virus. “Cases” are not people – they are technical curiosities or statistics. This technical language could do with some attention.
Invasive practices
High-quality and efficient testing is essential to understand and address the movement of the virus. In the early days of the public health response, there was good evidence for using nasopharyngeal swabs. However there are now far less invasive testing methods. One of the first locations to experience transmission was a dementia-care facility in Christchurch. At the time, the Director General of Health stated that the remainder of the residents would not be tested because the test was invasive, and they were not in a position to provide informed consent.
This is one of the few public acknowledgements that nasopharyngeal swabs are invasive, but they are widely considered to be. We have heard many unsolicited first-hand accounts of the fear of being tested, the anxiety of waiting to be tested and receiving a result, and awful experiences of the test itself. If we want people to be tested, we need to do better than this.
. . . talking about people who have tested positive as ‘cases’ has the tendency to define them as curiosities and other than human.
Use of saliva testing has been debated at length in Aotearoa New Zealand, with experts contributing opinions about its sensitivity.9,10 Regardless of the tensions between experts and interest groups, the invasive nature of nasopharyngeal swabs will be contributing to the reluctance of at least some people to be tested. Added to these fears is people’s general fatigue with restrictions and their impact on wellbeing. People need to be listened to and we need a less invasive test for at least the majority of people and settings.
The United Kingdom is promoting regular rapid lateral flow tests for people without symptoms. A clear distinction is made between testing for those with symptoms, for which the PCR (polymerase chain reaction) test is used, and routine testing for those without symptoms.
Testing is accessible and normalised. People order free testing kits, provide the required sample, and wait for a result that arrives in the form of a QR code. This enables people to travel and interact more freely and provides a level of reassurance, as well as contributing to ongoing routine surveillance of the virus.
The United Kingdom is promoting regular rapid lateral flow tests for people without symptoms . . . Testing is accessible and normalised.
In other countries, there are trials underway where double-vaccinated workers undergo at least daily non-invasive testing, allowing them to work without PPE and with only minimal public health limitations.
Using more invasive testing techniques will have an impact on the choices that at least some of the population make about being tested. For those who are expected to be tested regularly (drivers crossing “borders” between levels of restrictions, border workers and staff in high-risk settings) there is a humane and ethical obligation to choose a testing approach that balances the level of invasiveness with the sensitivity of the test.
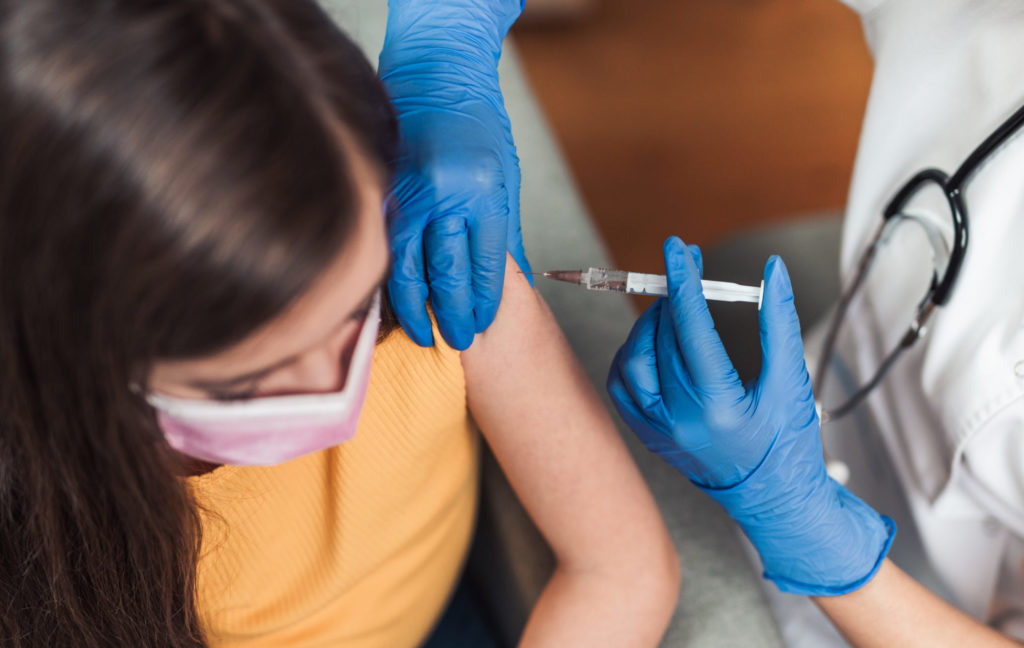
We are aware of the impact of misinformation on those accessing vaccination, but there will also be a proportion of the population who find vaccinations particularly invasive. In addition to the images conjured up by the language of “shot” and “jab”, a proportion of any population are fearful of needles or concerned about the procedure.11,12,13
There are many variables, for patient and vaccinator, that affect the pain of vaccination. The person giving the vaccination has control over their technique14 and also their interaction with the patient. As we have listened to people talk about their experiences, it is clear there are many factors at play. Our personal experience, and that of close family members, reveals a wide range of techniques. We have felt grateful each time someone who was anxious about being vaccinated has told us they were treated with kindness and that it made a difference for them.
When giving vaccinations, we need to consider the size of the needle relative to the patient and technique, because it is our responsibility to limit the discomfort we cause patients.15 We also need to be mindful that there are other techniques for administering vaccinations.16,17,18 While they are not tested or necessarily suitable for use with the current COVID-19 vaccinations, they are less invasive ways19 of administering at least some formulations that have previously been at the end of a sharp needle.
Invasive images
People receive messages through various routes. The mainstream media is constantly presenting graphic images of testing and vaccination. The images of people being tested are confronting and we have been interested to hear colleagues from the health sector talk about how shocking they are.
Likewise, the images of vaccination raise concerns. We have questions about the techniques that see syringes being wielded in all manner of ways, the skin being pierced abruptly and at great speed, and the clear discomfort some people in these images display as the needle is withdrawn.
Nasopharyngeal swabbing and vaccinations are invasive, and we need to be honest about that. Efforts to encourage relatively small numbers of people who are reluctant to engage are likely to be undermined by images that convey discomfort.
Conclusion
COVID-19 has invaded our lives in many ways. Restrictions have had an impact on relationships, incomes, wellbeing and the futures of many. Health professionals have an ethical obligation to consider how we engage with the invasive procedures that are at the heart of the public health response. We have the capacity, on a daily basis, to reconsider our language and practice to limit the references to violence and the pain and discomfort people experience.
Reducing the stress for people around testing and vaccination is likely to also de-escalate some of the stress among staff. In this way, we acknowledge our own wellbeing and ensure kindness remains at the centre of our response. We also need to remember to stay focused on equality and what true access and engagement looks like, because everything we do (and how we do it) really matters.
Susan Shaw, RN, MEdAdmin, EdD, Dip Tchg, PFHEA, is associate dean (academic) in the Faculty of Health and Environmental Sciences, at the Auckland University of Technology, responsible for curriculum, teaching, and learning across a range of disciplines serving the health and disability sector.
Rain Lamdin, MBChB, PhD, works as a doctor in emergency medicine in the public hospital system and an academic in clinical education at the University of Auckland.
References
- Graham, R., & Masters-Awatere, B. (2020). Experiences of Māori of Aotearoa New Zealand’s public health system: a systematic review of two decades of published research. Australia and New Zealand Journal of Public Health, 44(3), 193-200. https://doi.org/10.1111/1753-6405.12971
- Arnold, T. C. (2020). Moral distress in emergency and critical care nurses: A metaethnography. Nursing Ethics, 27(8), 1681-1693. https://doi.org/10.1177/0969733020935952
- Danesh, M. K., Garosi, E., & Golmohamadpour, H. (2021). The COVID-19 pandemic and nursing challenges: A review of the early literature. Work (Preprint), 1-14.
- Adcock, A., Stevenson, K., Cram, F., MacDonald, E. J., Geller, S., Hermens, J., & Lawton, B. (2021). He Tapu Te Whare Tangata (sacred house of humanity): Under‐screened Māori women talk about HPV self‐testing cervical screening clinical pathways. International Journal of Gynecology & Obstetrics, 155, 275-281. https://doi.org/10.1002/ijgo.13873
- Carter, B. S. (2021). Change the Language. Clinical Pediatrics, 60, (4-5), 201. https://doi.org/10.1177/0009922821998491
- Semino, E., Demjén, Z., & Demmen, J. (2018). An integrated approach to metaphor and framing in cognition, discourse, and practice, with an application to metaphors for cancer. Applied Linguistics, 39(5), 625-645. https://doi.org/10.1093/applin/amw028
- Dada, S., Ashworth, H. C., Bewa, M. J., & Dhatt, R. (2021). Words matter: political and gender analysis of speeches made by heads of government during the COVID-19 pandemic. BMJ Global Health, 6(1), e003910. http://dx.doi.org/10.1136/bmjgh-2020-003910
- Wood, J. D., & Griffin, P. M. (2021). The policing and public health interface: insights from the COVID-19 pandemic. Policing and Society, 31(5), 503-511. https://doi.org/10.1080/10439463.2021.1946058
- Atieh, M. A., Guirguis, M., Alsabeeha, N. H., & Cannon, R. D. (2021). The diagnostic accuracy of saliva testing for SARS‐CoV‐2: a systematic review and meta‐analysis. Oral Diseases. https://doi.org/10.1111/odi.13934
- Wyllie, A. L., Fournier, J., Casanovas-Massana, A., Campbell, M., Tokuyama, M., Vijayakumar, P., Warren, J. L., Geng, B., Muenker, M. C., Moore, A. J., Vogels, C. B. F., Petrone, M. E., Ott, I. M., Lu, P., Venkataraman, A., Lu-Culligan, A., Klein, J., Earnest, R., Simonov, M., Datta, R., Handoko, R., Naushad, N., Sewanan, L. R., Valdez, J., White, E. B., Lapidus, S., Kalinich, C. C., Jiang, X., Kim, D. J., Kudo, E., Linehan, M., Mao, T., Moriyama, M., Oh, J. E., Park, A., Silva, J., Song, E., Takahashi, T., Taura, M., Weizman, O.-E., Wong, P., Yang, Y., Bermejo, S., Odio, C. D., Omer, S. B., Dela Cruz, C. S., Farhadian, S., Martinello, R. A., Iwasaki, A., Grubaugh, N. D., & Ko, A. I. (2020). Saliva or nasopharyngeal swab specimens for detection of SARS-CoV-2. [Letter to editor]. New England Journal of Medicine, 383(13), 1283-1286.
- MacDonald, N. E., Butler, R., & Dubé, E. (2018). Addressing barriers to vaccine acceptance: an overview. Human vaccines & immunotherapeutics, 14(1), 218-224.
- Taddio, A., McMurtry, C. M., Shah, V., Riddell, R. P., Chambers, C. T., Noel, M., MacDonald, N. E., Rogers, J., Bucci, L. M., Mousmanis, P., Lang, E., Halperin, S. A., Bowles, S., Halpert, C., Ipp, M., Asmundson, G. J. G., Rieder, M. J., Robson, K., Uleryk, E., Antony, M. M., Dubey, V., Hanrahan, A., Lockett, D., Scott, J., Bleeker, E. V., & HELPinKids&Adults. (2015). Reducing pain during vaccine injections: clinical practice guideline. Canadian Medical Association Journal, 187(13), 975-982. https://doi.org/10.1503/cmaj.150391
- Ventola, C. L. (2016). Immunization in the United States: recommendations, barriers, and measures to improve compliance: part 2: adult vaccinations. Pharmacy and Therapeutics, 41(8), 492-506.
- Petousis-Harris, H., Poole, T., Stewart, J., Turner, N., Goodyear-Smith, F., Coster, G., & Lennon, D. (2013). An investigation of three injections techniques in reducing local injection pain with a human papillomavirus vaccine: a randomized trial. Vaccine, 31(8), 1157-1162. https://doi.org/10.1016/j.vaccine.2012.12.064
- Shaw, S., & Lamdin, R. (2011). Nurses have an ethical imperative to minimise procedural pain. Kai Tiaki Nursing New Zealand, 17(7), 12-14.
- Arya, J., Henry, S., Kalluri, H., McAllister, D. V., Pewin, W. P., & Prausnitz, M. R. (2017). Tolerability, usability and acceptability of dissolving microneedle patch administration in human subjects. Biomaterials, 128, 1-7.
- Fernando, G. J., Hickling, J., Flores, C. M. J., Griffin, P., Anderson, C. D., Skinner, S. R., Davies, C., Witham, K., Pryor, M., Bodle, J., Rockman, S., Frazer, I. H., & Forster, A. H. (2018). Safety, tolerability, acceptability and immunogenicity of an influenza vaccine delivered to human skin by a novel high-density microprojection array patch (Nanopatch™). Vaccine, 36(26), 3779-3788.
- Hettinga, J., & Carlisle, R. (2020). Vaccination into the dermal compartment: techniques, challenges, and prospects. Vaccines, 8(3), 534. https://doi.org/10.3390/vaccines8030534
- O’Shea, J., Prausnitz, M. R., & Rouphael, N. (2021). Dissolvable microneedle patches to enable increased access to vaccines against SARS-CoV-2 and future pandemic outbreaks. Vaccines, 9(4), 320.