Simulation is an effective training tool in a wide variety of settings. Shifting from a clearly simulated environment to a more realistic scenario, similar to what a nurse may encounter in the ward, offers the opportunity take full advantage of this powerful training tool.
Currently the Nursing Council limits the use of simulation to augment clinical hours.1 But using ultra-realistic simulations, training for rare, dangerous or expensive scenarios can be facilitated in a straightforward manner, while simultaneously closing the theory-practice gap.
Ultra-real simulations are often used in the military, where recruits are put into high-pressure simulation. This approach allows the recruits to gain the practical skills necessary for the work and also gives an idea of the mental and emotional strain experienced on the battlefield. Experiencing this stress in a controlled environment allows for a structured debriefing and an assessment of individual recruits’ coping mechanisms. This simulated experience also provides experience in dealing with trauma, both clinically and emotionally.
Multiple-patient simulations
There is a growing realisation that including high-fidelity simulation in undergraduate nursing education can better prepare nurses for their working environment.2 The protocols and standards for implementing single-patient scenarios are well established. However, developing a simulated environment focusing on just one simulated patient, limits this powerful learning tool. For example, the emergency department (ED) can be a chaotic environment – and a primary source of that chaos is managing multiple patients simultaneously, not just a single patient. Simulated training for the ED and disaster response should include caring for multiple patients simultaneously to reflect this reality.
The challenge with ED workflow is, primarily, the simultaneous triage and management of multiple patients with a range of needs.3 Simulations involving a number of patients are a much more realistic representation of a typical ED nurse’s day than a simulation focusing on one individual case. Ideally, the simulation would include a comprehensive, ED-based simulation with multiple patients.4 Simulations involving a number of patients enable specific incidents or tasks to be developed to test nursing competencies. These would be impossible to assess didactically and challenging to assess in a traditional supervised training environment. For example, delegation and prioritisation of patient load can both be accurately assessed in this simulated environment.4, 5 Clearly this type of multi-patient simulation is not limited to the ED and the approach could be refined to reflect any practice specialty.5
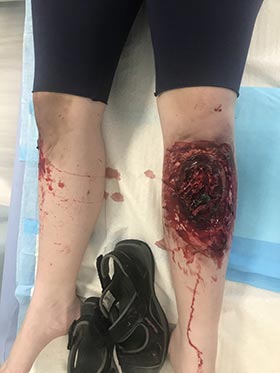
It is essential these educational simulations mimic reality. This can include creating life-like injuries that replicate the injuries that would be expected to occur in the event being simulated. Specifically that could entail glass fragments from a car accident, exposed bone in a severe fracture or brain injury in the case of a fall.
Volunteer actors
The educational power and value of simulation training is its ability to mimic reality. Thus, rather than manikins as patients, there may be value in including actor volunteers from the local amateur dramatic society or from arts programmes at the local university, technical institute or school. In the case of acting students, part of their training could be learning and incorporating the different symptoms of the assigned disorder, to increase the psychological fidelity of the training and its association with real-world consequences.6 Video recording the actors and nurses would provide all participants with a valuable resource to assess both their nursing and acting performance.
There is no doubt that implementing individual patient simulations is a good training technique for nurses. But the real value in simulations is being able to simulate the truly testing environments that occur on wards and the complex, multi-faceted management that needs to occur for patient care. These simulations need to be focused and realistic, with minimal facilitator input and direction once the scenario is running. This style of learning in a safe environment, with effective and extensive feedback, is a powerful learning tool7 – and we have also found it to be great fun for all the participants.
Andy Redpath, RN, is a lecturer in the school of nursing at Manukau Institute of Technology.
References
- Nursing Council of New Zealand. (2015). Education programme standards for the registered nurse scope of practice.
- Truchot, J. (2020). Point of care simulation: towards new pragmatic simulation training. European Journal of Emergency Medicine, 27, 79-80. doi: doi.org/10.1097/MEJ.0000000000000682.
- Davies, H., Jacob, E., Schultz, R., & Sundin, D. (2020). Ward for the day: A case study of extended immersive ward-based simulation. Nurse Education Today, 90. doi.org/10.1016/j.nedt.2020.104430.
- Sullivan, N., Swoboda, S. M., Breymier, T., Lucas, L., Sarasnick, J., Rutherford-Hemming, T., & Kardong-Edgren, S. (2019). Emerging Evidence toward a 2:1 Clinical to Simulation Ratio: A Study Comparing the Traditional Clinical and Simulation Settings. Clinical Simulation in Nursing, 30, 34-41. doi.org/10.1016/j.ecns.2019.03.003.
- Gamble, A. S. (2019). Simulation in undergraduate paediatric nursing curriculum: Evaluation of a complex ‘ward for a day’ education program. Nurse Education in Practice, 23, 40-47. doi.org/10.1016/j.nepr.2017.02.001.
- de Oliveira, S. N., do Prado, M. L., Kempfer, S. S., Martini, J. G., Caravaca-Morera, J. A., & Bernardi, M. C. (2015). Experiential learning in nursing consultation education via clinical simulation with actors: Action research. Nurse Education Today, 35, 50-54. doi.org/10.1016/j.nedt.2014.12.016.
- Berglund, M., Pettersson, A., & Sundler, A. (2015). Undergraduate nursing students’ experiences when examining nursing skills in clinical simulation laboratories with high-fidelity patient simulators: A phenomenological research study. Nurse Education Today, 35, 1257-1261. doi.org/10.1016/j.nedt.2015.04.008.



