Recommendations
- Prioritise growth of the Māori nurse academic workforce and the Pacific nurse academic workforce with clear pathways.
- Establish a clear academic nurse career pathway for registered nurses as an advanced practice nursing role (reflecting parity to clinical advanced nursing practice). This development would consider nurse academia as an area of specialty practice.
- Align salary and working conditions for nurse academics with nurses in clinical practice.
Academics — nurses working in tertiary education — take at least 10 years to train and make up just 1.5 per cent of the nursing workforce. But they were crucial to fostering a clinically and culturally competent workforce, as well as research-informed practice, teaching and curricula, group spokesperson Kathy Holloway said in a statement.
The group represented all 20 schools of nursing in Aotearoa — Te Pūkenga, universities and wānanga — and about 1000 staff, she said. Joining forces to speak up was an unprecedented move, driven by the high level of concern, Holloway told Kaitiaki Nursing New Zealand.
Recent job cuts across universities and Te Pūkenga, alongside a growing pay gap with nurses in clinical practice, had put the academic workforce under threat, said Holloway, who is head of nursing, midwifery and health science at Victoria University of Wellington.
“Current funding cuts across the tertiary sector result in increased workload, burnout, emotional fatigue and frustration as staff navigate to support the health sector workforce,” she said.
The challenges had been exacerbated after the NZNO-Te Whatu Ora collective agreement, which made it “even harder to attract nurses into academia due to increasing pay inequities”, Holloway said.

She said in 2022, salaries began at around $80-100,000 for an entry-level nursing lecturer role — sometimes even less at Te Pūkenga. This compared to $96-144,000 for an equivalent senior nurse working for a then-district health board. Under the new NZNO-Te Whatu Ora collective agreement, the gap would be even wider.
Having fewer educators would impact on numbers of sorely-needed nursing graduates in Aotearoa, she warned.
“Any exacerbation of nurse academic shortages at nursing schools across the country will limit student capacity at a time when the need for registered nurses continues to grow.”
Research was the “backbone” of nursing education and was primarily led by nursing programme providers, she said. “Without sufficient nursing staff . . . there is the risk of missing opportunities for nursing innovation and population-facing health responses.”
‘To attract Māori students into nursing, we need Māori educators and academics to provide education, lead and promote research, influence system changes and inspire the next generation of nurses to improve health care for all people in Aotearoa New Zealand.”
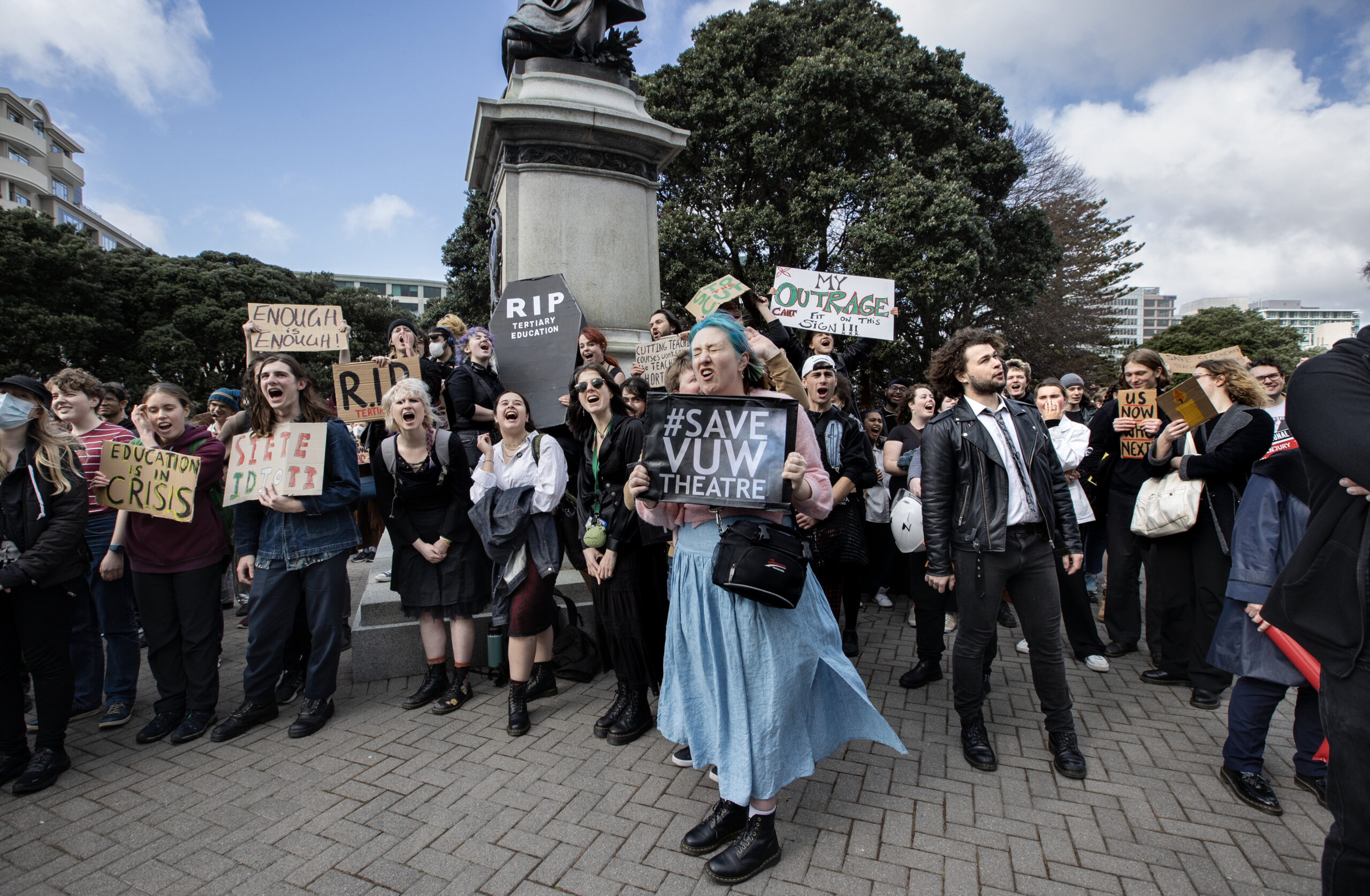
‘Urgent’ support for Māori, Pacific needed
The group wants urgent support to increase Māori and Pacific nurse educators, clearer pathways for all registered nurses (RNs) into academia and more aligned salaries and working conditions to peers in clinical practice.


Just three per cent of the nurse academic workforce identify as Māori or Pacific.
Co-chairs of Wharangi Ruamano, which represents Māori nurse and midwife educators, Jan Dewar and Zoe Tipa, said it was important to increase the number of Māori educators. This would “ensure nursing schools are equipped with the cultural insight and expertise to develop the cultural safety of all students when caring for whānau Māori”.
Māori nurse numbers — seven per cent of the workforce compared to a population of 15 per cent — needed to increase to match population need and bring equity to health experiences and outcomes for Māori, said Dewar and Tipa. Dewar is head of nursing at Auckland University of Technology and Tipa is chief nurse at Whānau Āwhina Plunket — both hold doctorates.
“To attract Māori students into nursing, we need Māori educators and academics to provide education, lead and promote research, influence system changes and inspire the next generation of nurses to improve health care for all people in Aotearoa New Zealand.”
Whitireia’s Pacific nursing head Tania Mullane said Pacific nursing educators were essential to running Pacific nursing programmes to ensure their “essence, philosophy and intent” was maintained.
“Indigenised” programmes such as the BN Pacific brought a Pacific lens to, not only cultural, but academic and professional aspects of the programme, through “who teaches them, how they are taught and where they are taught”.

The “severe” pay disparity deterred Pacific nursing graduates from becoming educators, said Mullane, who estimates there were only about 25 Pacific nurse educators currently.
Whitireia was “incredibly lucky” to have Pacific nurses willing to work part-time as educators on top of full-time clinical roles, she said.
The need for more locally-trained nurses, particularly in under-represented communities like Māori and Pacific was identified in the recent health workforce plan.
Holloway said the goal of nurse academics was, through education and research, to support “safe, confident, competent, clinically and culturally competent registered nurses for Aotearoa at both the undergraduate and post-graduate levels”. They also supported post-graduate development of nurses across clinical, management, leadership, education and research areas.
The group comprises Wharangi Ruamano, the Council of Deans of Nursing and Midwifery (Australia and New Zealand), and Nurse Education in the Tertiary Sector.
The Minister of Health Ayesha Verrall referred Kaitiaki to Te Whatu Ora, which was not able to provide a response by deadline.




