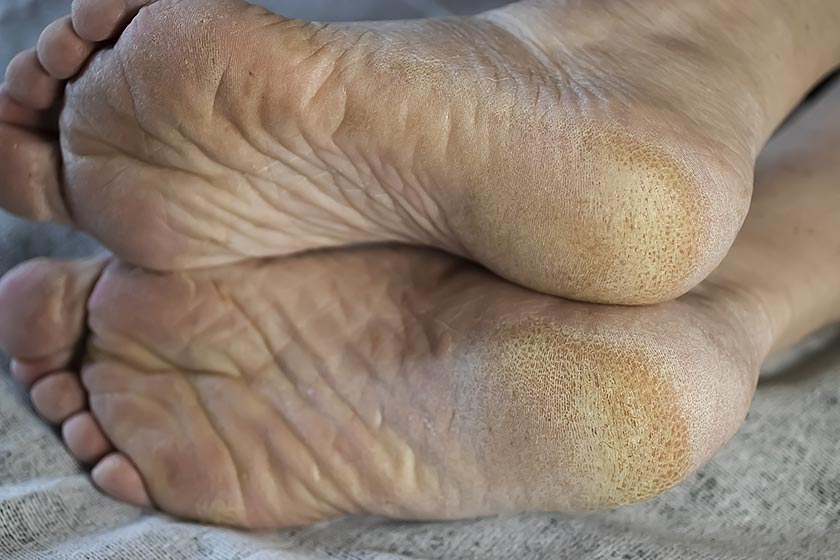
Foot care is an important part of personal care, and registered nurses (RNs) are in a pivotal position1, 2 to help meet this care need for our ageing population.3 As leaders in assessment and care planning, RNs are in a position to make a substantial difference to the health, wellbeing and safety of patients.
Elderly, diabetic, and/or disabled patients often present with foot conditions which they find difficult to manage and may initially look to primary health care services for information regarding how best to care for their feet. It is important that RNs recognise the importance of foot health.
Any changes in feet, nails and skin of patients with diabetes should be assessed and treated as soon as possible.6
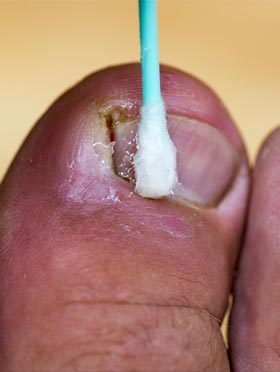
“Foot care is a very important part of personal care, especially for those who are unable to care for their own feet due to comorbidity such as diabetes, or advanced age.”4 Anyone who has damaged their own toe will know, foot hygiene and health is important for a sense of well-being and has a significant impact on comfort and mobility.
Research makes it clear that 80 percent of people over the age of 80 find managing their toenails difficult.2 This may be due to poor eyesight, poor balance, reduced flexibility, arthritis, obesity, shortness of breath, pain, tremor, weak hand muscles, dizziness or other chronic health conditions such as diabetes3 or rheumatoid arthritis.4
They may have problems with overlapping toes, tenderness or open areas. Nails may also present problems with shape, thickness, fungal infection or edges that are prone to in-grow. Previous injury to feet, toes or nails can also make them difficult to manage.
When foot care is lacking
When a patient doesn’t get the foot care they need, these are some of the problems that may result:
Pain: The patient may suffer pain from long nails dragging on sheets, carpet, socks or shoes. Long toenails may be digging into the toes. Corns or calluses may be present on the toes or soles, making each step a challenge.
Reduced mobility: This pain can result in reduced or unstable mobility, which can negatively affect quality of life, independence, exercise, concentration, demeanor and mood.
Injury: Long toenails can cut either the underside of the toe if they curl under, or the side of an adjacent toe.
Accidental injury: People can accidentally cut their toes when they are trying to cut their toenails. These injuries can become infected, or in the case of patients with diabetes1 extremely difficult to heal. Any changes in feet, nails and skin of patients with diabetes should be assessed and treated as soon as possible.6
In extreme cases, gangrene can become established if circulation to the feet and toes is compromised, resulting in amputations that could have been avoided.
What you can do to help
There are a number of simple, practical ways to assist with foot care. Number one is regular assessment of the feet of people with diabetes6 (or patients who complain about painful feet, nails, or other related issues).
After assessing the patient’s feet, nurses can then plan foot care, monitoring and guidance. This may include advocating regular professional foot care or referral to a specialist foot-care provider.
You should ask elderly and disabled patients how they manage their foot and nail care, undertake a general assessment, and discuss ongoing management options with them. Patients will usually not raise the subject themselves.
Foot-care services in the community include podiatry clinics, community foot-care clinics, beauty therapy clinics, and visiting RNs providing basic care in the home. Clients may need help from a GP or practice nurse6 to access podiatry services or get contact details for foot-care services.
Foot assessment
Any initial assessment by an RN7 of feet and nails should include contact details, clinical history and expectations. Examine skin, feet, toes and legs for colour, oedema, inflammation, deformity, pain, evidence of disease or injury and skin integrity, fragility and elasticity. Examine nails for pain, thickness, brittleness, shape, contour, colour and infection. Discuss a plan of care with the client, covering immediate needs and ongoing care of their feet and nails.
All patients with diabetes should have annual foot assessment to identify changes in sensation or circulation. If either is identified then it is recommended that foot care is provided by a podiatrist. Most DHBs have subsidised podiatric care for patients with high-risk feet related to peripheral vascular disease or peripheral neuropathy.
Basic foot care includes:
- Trimming and filing of toenails.
- Reduction of corns and calluses.
- Cleaning and dressing of any open areas/wounds.
- Sanitiser with moisturiser applied to feet and toes.
- Cream may be massaged into dry skin.
- Fingernails may be cut and filed alongside foot care, if requested by the client and/or offered by the service provider.
Ongoing care can include follow-up appointments at either four, six, eight or 12-week intervals, depending on what the client needs, or a client may be directed to a mobile foot-care community clinic.
Cost
The cost of foot care may range from $55 per visit with a RN to $105 with a podiatrist, or $30 at a community clinic run by an RN. Clients with diabetes can access some conditional free foot care from a podiatrist via a GP referral. WINZ may reimburse foot-care costs using the disability allowance via receipt.
ACC and Veterans Affairs will provide free foot care with a GP referral.
Foot-care services are currently being reviewed in some regions,4 though without plans to use RNs. Podiatrists have recently demonstrated their support of nurses providing basic foot care by issuing a “Guide for providers of basic foot care who are not registered podiatrists”. More nurses are acknowledging the importance of foot care, and becoming interested in providing it.
Podiatrists are acknowledging and discussing the value of a “second tier” foot-care provider, as their numbers dwindle, and the need for foot care increases.
RN education
The Ontario College of Health Studies in Canada has a well-established Foot Care Nurse Association and offers online education9 to RNs and NPs worldwide.
I am exploring options for the establishment of consistent post graduate foot-care education for nurses in New Zealand.
Heather Woods, RN, BN, DipCouns, CmtyCert PsychCare, is a clinical nurse specialist, who has run a private practice foot clinic in North Canterbury for 30 years.
Kaiapoi RN has foot in community care

I am a registered nurse (RN) based in North Canterbury, and for the past 30 years I have run my own primary health care foot clinic, Mobile Foot Care.
Referrals for affordable foot care come to me from GPs, practice nurses, carers, families and podiatrists, and I provide this service both in my clinic and in people’s homes.
My journey towards setting up and managing Mobile Foot Care Ltd started when I injured my back nursing and wanted the kind of practice where I could sit down to work. I am also passionate about the importance of foot care.
I invested time and money to prepare for the role by working for a year with a podiatrist as a foot- care assistant. I learned basic foot care, including care of nails, corns and calluses. The podiatrist was enthusiastic and supportive of an RN providing a low-cost, mobile, domiciliary service. He could see the need for it and believed podiatrists would not be interested in providing such a service. I would refer clients needing advanced care back to him.
There is certainly benefit in an RN providing this service – bringing with them nursing knowledge, assessment skills and nursing philosophy. As an RN, I can also assess, plan, evaluate and understand needs or behaviours related to physical, psychiatric, neurological and sensory disabilities, and to intellectual disability or dementia.
While preparing to start my service, I also completed a person-centred counselling diploma at the then Christchurch Polytechnic. This fine-tuned my ability to listen and respond during the inevitable conversations which arise during home visits.8 Broader health-related questions often arise, providing the opportunity for health education and if required, referral to a GP, nurse practitioner (NPs), or other primary health service.
I provide home visits
A home visit by a friendly, professional RN is often as valued by the client as much as the foot care. Patients have reported a feeling of total wellbeing following the consultation, not just the fact that their feet feel much better. Older people are often lonely and a friendly regular visit can ease their isolation.
Community foot-care clinics

At the request of a rural GP, I set up four community foot-care clinics in Canterbury where basic foot/nail care is provided. I run them monthly for a minimal charge, and regular appointments are kept.
Recently I trained three RNs who have all set up their own foot care companies; set up five more community clinics; and also provide home visits. I am the central contact for anyone in Canterbury seeking foot care, and refer them to the nurse in their area. So my role has moved towards coordination and support as I age.
Foot care involves liaison between many health professionals, including GPs, practice nurses, NPs, district nurses, hospitals, occupational health, palliative care, ACC, aged and residential care facilities, podiatrists, chemists, carers, beauty therapists, emergency care workers, diabetes staff, elderly day-care staff and social services. Nurses have a pivotal role in coordinating and planning this care.6
References
- Daly, B., Arroll, B., Sheridan, N., Kenealy, T., Stewart, A., & Scragg, R. (2014). Foot examinations of diabetes patients by primary health care nurses in Auckland, New Zealand. Primary Care Diabetes, 8(2), 139-146.
- Peterson, J. M., & Virden, M. D. (2013). Improving diabetic foot care in a nurse‐managed safety‐net clinic. Journal of the American Association of Nurse Practitioners, 25(5), 263-271.
- University of Auckland. (2017). Report finds our aging population will need increased levels of care.
- Waitemata District Health Board. (2018).
- Harvey, I., Frankel, S., Marks, R., Shalom, D., & Morgan, M. (1997). Foot morbidity and exposure to chiropody: population based study. BMJ, 315(7115), 1054-1055.
- Keller-Senn, A., Probst, S., Imhof, R. M., & Imhof, L. (2015). Nurse-led education programme enhancing foot care self-efficacy in high-risk diabetes population: pilot randomised controlled study. International Diabetes Nursing, 12(2), 74-78.
- Rome, K., Gow, P. J., Dalbeth, N., & Chapman, J. M. (2009). Clinical audit of foot problems in patients with rheumatoid arthritis treated at Counties Manukau District Health Board, Auckland, New Zealand. Journal of Foot and Ankle Research, 2(1), 16.
- New Zealand Nursing Review. (2014). Faith, duty and foot pampering wins nurse QSM. New Zealand Nursing Review, 14(3), 15.
- College of Health Studies. (2018). Basic and Advanced Nursing Foot care Competencies and Standards.
This article was reviewed by Waitemata District Health Board diabetes clinical nurse specialist Lisa Sparks.