Many human viral diseases result from a zoonotic event (transfered from an animal). Some of these diseases have affected millions of people around the world, and some have resulted in high rates of morbidity/mortality in humans.
Zoonotic outbreaks over the last two decades include severe acute respiratory syndrome (SARS-CoV) in 2002, MERS-CoV in 2012, Ebola virus in 2014 and, in December 2019, a world outbreak of a novel coronavirus (SARS-CoV-2). This initially emerged in a wholesale seafood market in Wuhan, China, with bats the likely original hosts and pangolins as potential intermediate hosts.1
SARS-CoV-2 is the etiologic agent of coronavirus disease 2019 (COVID-19), which causes severe respiratory illness in humans. Based on current evidence, it is transmitted through close contact and droplets, as previously seen in SARS-CoV and MERS-CoV. Airborne transmission may also occur during aerosol-generating procedures. It was recognised as a pandemic by the World Health Organization (WHO) in March 2020 and has had considerable global economic and health impacts.2, 3 This pandemic has also highlighted the vulnerability of health-care workers to respiratory infections.
A major challenge in every pandemic is the effective protection of health-care workers as they are at risk of infection themselves. Health-care workers use personal protective equipment (PPE) to protect themselves from droplets from coughs, sneezes or other body fluids from infected patients and contaminated surfaces that might infect them. Recommendations for the use of PPE to protect against SARS-CoV-2 exposure by health-care workers were recently published by the WHO and the United States Centers for Disease Control and Prevention (CDC).
There are questions regarding the effectiveness of PPE as an infection control strategy to protect health-care workers during the COVID-19 pandemic and other epidemics. Does it lead to an increased, rather than decreased, risk of infection among health-care workers if proper selection, fit, sequence for donning and doffing or adequate training is not implemented? This includes correct and consistent use, disposal, disinfection and maintenance.
Risks to health-care workers
Health-care workers are at the front-line in every pandemic and epidemic outbreak. Their constant exposure to infected patients and contaminated surfaces can put them at risk of acquiring the infection. One study showed that procedures capable of generating aerosols have been associated with increased risk of virus transmission to health-care workers.4
During the 2002-2003 SARS epidemic, approximately 1725 front-line health-care workers were infected. During the COVID-19 pandemic, it was estimated that from December 2019 to February 2020, 1716 Chinese health-care workers were infected by COVID-19 and five died.5, 6 In Lombardy, Italy, the number of positive health-care workers was 10,627, with 34 deaths to date. Deaths among health-care workers in the United Kingdom (UK) were seven as of April 2020.7 During the Ebola virus outbreak in West Africa in early 2013 to 2016, a high proportion of infections were among health-care workers.8, 9
Infection among health-care workers during the aforementioned pandemics and epidemics were attributed to PPE shortages, incorrect PPE, inconsistent use of PPE, inadequate fit testing, insufficient training with donning and doffing, suboptimal hand hygiene before and after contact with patients, and protocol failure.6, 7, 8, 9, 10
Specific requirements for health-care workers’ protection are advisable to ensure the functioning of the health-care system. Understanding the transmission risk is particularly important for guiding evidence-based protective measures in health-care settings.11
Knowledge and practice gaps
PPE use is aimed at preventing transmission of these viruses from patients to health-care workers and vice versa, particularly when no effective treatment or prophylaxis is available. PPE includes gloves, surgical face masks, goggles or face shields and isolation gowns, as well as N95 respirators for aerosol-generating procedures.12
During a pandemic and epidemic, correct PPE use is crucial. As health-care workers frequently need to use several types of PPE, issues arise regarding the integration and interface of these items to ensure they provide the best protection and that contamination is avoided.13 Findings from the literature have shown that even the best-designed and engineered PPE will not protect health-care workers if it is not selected appropriately, is unreliable or unusable due to incorrect fit, inconsistent use and training in the proper sequence for donning and doffing, and disposal or maintenance is insufficient.7, 8, 9, 15
A number of randomised control trials and studies show that inconsistent use of PPE, insufficient training and inadequate fit of masks can put health-care workers at risk of infection such as COVID-19 and other viruses. In a randomised control trial, health-care workers who wore surgical masks or N95s throughout their work shift were significantly protected against nonspecific respiratory infection, compared to those who did not. However, assessment of clinical outcomes was self-reported and prone to bias, as the intervention cannot be masked.15
Dangers of insufficient training
Evidence from a cohort study conducted among health-care workers in Hong Kong and Toronto showed that insufficient training in and inconsistent wearing of either a surgical mask or an N95 was associated with developing SARS when compared with sufficient training and consistent use.10 The efficacy of respiratory protection in preventing respiratory infection among health-care workers may easily be lost, if compliance is poor or insufficient training is provided. Other studies have shown that inadequate fit of masks could compromise respiratory protection and impair vision, due to masks moving on the face. Continuously touching the mask, even with gloved hands to adjust it, can result in self-inoculation when the health-care worker inadvertently touches their face, eyes, nose or mouth. Some volunteers wore glasses which steamed up, showing further evidence of poorly-fitted masks.8, 13
Recent studies, simulations and reviews have examined the dangers to health-care workers during PPE removal. This is when the risk of contamination is highest. Researchers found that the sequence of PPE removal, complication or error in doffing, protocol failure, hand-hygiene compliance, problems with protection, comfort and function were significant factors in contamination of health-care workers. An observational study performed in 11 hospitals in Canada found that only half the health-care workers removed their PPE in the correct sequence and hand hygiene was not routinely performed after PPE removal, thereby creating opportunities for self-contamination.14 In a UK study in 2018, researchers saw that the health-care workers were frequently contaminated, either through a protocol failure of the PPE ensemble itself, complication or errors in doffing.8
The provision of PPE has limited benefit and is only one strategy within a hierarchy of infection prevention and control measures.
A recent experimental simulation of intubation was conducted by researchers using fluorescent-simulated body fluid. This demonstrated contamination of the air in the breathing zone of participants and on the gloves, gowns (torso and cuffs) and face shields of participants.16 Another study evaluated seven PPE ensembles designed for use for highly infectious diseases using a human factors lens. This found problems with protection, comfort, function during simulated care activities and doffing, which is similar to a 2020 Cochrane systematic review.17 The review found there was low to very-low certainty evidence that covering more parts of the body led to better protection. Also, this usually comes at the cost of more difficult donning or doffing and less user comfort, and may therefore even lead to an increased risk of contamination when health-care workers remove it.18
Overall, the knowledge and practice gaps in the effective use of PPE shown in different studies, simulations, randomised trials and reviews strongly demonstrated that PPE may cause more harm than good and may contribute to an increased risk of having COVID-19 infection and other respiratory infections among health-care workers.
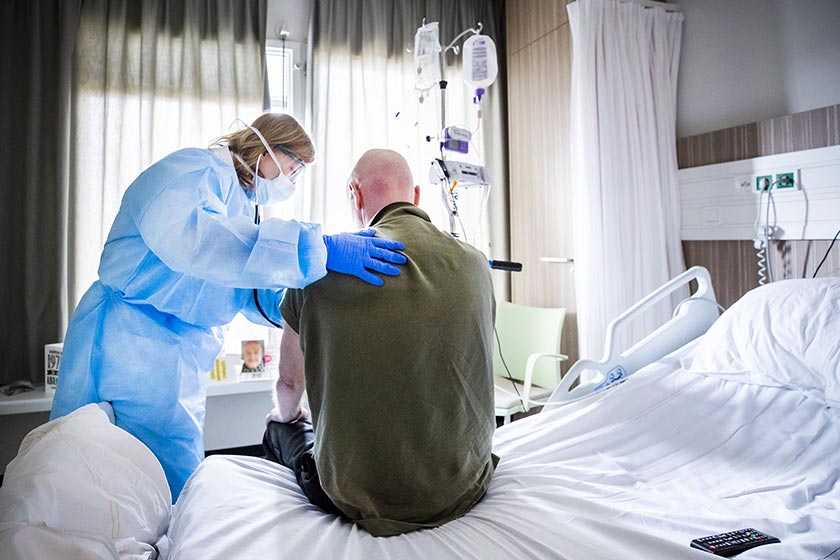
The proper use of PPE by health-care workers is vital in protecting them from biological hazards such as COVID-19 and other viruses. Fundamental is the selection of the correct PPE for each setting and context.12, 19, 20 The Health and Safety at Work Act 2015 legislates that an employer will provide suitable PPE for an employee in their work. The employee must also receive adequate education and training.21 The Ministry of Health, in line with the WHO guidelines, recommends the consistent use of PPE during exposure to biological hazards, the correct sequence of donning and doffing, performing hand hygiene after removal of any element of PPE and proper maintenance, disinfection or disposal of PPE.12, 19
One of the critical features in helping achieve consistency in wearing PPE may be the comfort and proper fit of the equipment itself.13 Multiple respirators should be available, because it is unlikely one model or size will fit all employees. Filtering facepiece respirators, including N95s, rely on having a good seal with the wearer’s face. Therefore, a face fit test and pre-use seal check or fit check should be carried out in compliance with the NZ Standard AS/NZS 1715:2009 to ensure the respiratory protective equipment can protect the wearer against biological hazards. This is supported by several studies.10, 19, 22 For correct donning and doffing procedures, CDC guidance provides a useful protocol.23 A one-step glove and gown removal, and hand hygiene after PPE removal can reduce contamination or self-inoculation.18
Increased compliance and reducing errors can be achieved by having detailed policies and protocols, personal supervision, spoken instructions during doffing, face‐to‐face education and training in PPE use rather than folder‐based training, checklists, audits of performance, providing feedback and allowing sufficient time for donning and doffing.9, 18
Buddy system for instruction
A lesson the UK military learned from deployment on Operation Gritrock during the Ebola virus epidemic was to have a donning and doffing supervisor. When this was not possible, a buddy-buddy system was used. This can reduce self-infection/cross-contamination and provides automaticity of safe and efficient donning and doffing of PPE among health-care workers.7 Qualitative feedback supported having a buddy present to instruct during doffing. This helped ensure fatigued staff followed the correct doffing procedure, bringing a personal approach rather than relying on instruction cards, ensuring protocol compliance or necessary intervention was followed, controlling the pace and providing calm reassurance. Ideally, the buddy should be an observer and instructor, but should not physically assist in doffing, to reduce the number of workers at risk of contamination.8, 9
In occupational health, the hierarchy of controls is best practice. This means that measures with a general effect, such as control of exposure, should have priority over more individual control measures such as PPE. The provision of PPE is only one strategy within a hierarchy of infection prevention and control (IPC) measures.8, 19, 21, 24 It should be used in combination with effective administrative and engineering controls, as described in the WHO’s IPC measures for epidemic and pandemic acute respiratory infections in health care.12
Conclusion
Health-care workers are at the front line during pandemics and epidemics, exposed to biological hazards that put them at risk of infection. To prevent acquiring infections such as COVID-19, the use of PPE remains critical.
Knowledge and practice gaps may exist in the effective use of PPE that can pose an increased risk of infection among health-care workers. Adequate education and training are vital to prevent compromising the efficacy of PPE or indeed self-contamination while incorrectly doffing it. In addition, the use of PPE in conjunction with other IPC measures among the hierarchy of controls is considered best practice where practicable.
Further systematic studies for effective use of PPE, focusing on optimal types of PPE against transmissible viruses, reengineering PPE, strategies for minimising transmission during the doffing process, and the disease transmission of viruses, especially COVID-19, are needed to ensure health-care workers’ safety.
This article has been reviewed by Tauranga Hospital IPC clinical nurse specialist Robyn Boyne and the co-editors.
Alex Pajel, RN, BN, is an occupational health nurse at OK Health Services/Habit Health in Christchurch. This article is based on a 2020 assignment for a postgraduate certificate in occupational health and safety at Otago University.
References
- Peeri, N. C., Shrestha, N., Rahman, M. S., Zaki, R., Tan, Z., Bibi, S., . . . Haque, U. (2020). The SARS, MERS and novel coronavirus (COVID-19) epidemics, the newest and biggest global health threats: what lessons have we learned? International Journal of Epidemiology. doi:10.1093/ije/dyaa033
- World Health Organization. (2020). Coronavirus disease 2019 (COVID-19): situation report, 72. Geneva: Author.
- World Health Organization (WHO). (2020). Modes of transmission of virus causing COVID-19: implications for IPC precaution recommendations.
- Tran, K., Cimon, K., Severn, M., Pessoa-Silva, C. L., & Conly, J. (2012). Aerosol generating procedures and risk of transmission of acute respiratory infections to healthcare workers: a systematic review. PloS one, 7(4), e35797-e35797. doi:10.1371/journal.pone.0035797
- Ran, L., Chen, X., Wang, Y., Wu, W., Zhang, L., & Tan, X. (2020). Risk Factors of Healthcare Workers with Corona Virus Disease 2019: A Retrospective Cohort Study in a Designated Hospital of Wuhan in China. Clinical Infectious Diseases, ciaa287. doi:10.1093/cid/ciaa287
- Surveillances, V. (2020). The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) – China, 2020. China CDC Weekly, 2(8), 113-122.
- Herron, J., Hay-David, A., Gilliam, A., & Brennan, P. (2020). Personal protective equipment and Covid 19-a risk to healthcare staff? The British Journal of Oral & Maxillofacial Surgery, 58(5), 500-502.
- Hall, S., Poller, B., Bailey, C., Gregory, S., Clark, R., Roberts, P., . . . Crook, B. (2018). Use of ultraviolet-fluorescence-based simulation in evaluation of personal protective equipment worn for first assessment and care of a patient with suspected high-consequence infectious disease. Journal of Hospital Infection, 99(2), 218-228. https://doi.org/10.1016/j.jhin.2018.01.002
- Honda, H., & Iwata, K. (2016). Personal protective equipment and improving compliance among healthcare workers in high-risk settings. Current Opinion in Infectious Diseases, 29(4), 400-406. doi:10.1097/qco.0000000000000280
- Gamage, B., Moore, D., Copes, R., Yassi, A., Bryce, E., & members of The B.C.I.R.P.S.G. (2005). Protecting health care workers from SARS and other respiratory pathogens: A review of the infection control literature. American Journal of Infection Control, 33(2), 114-121. https://doi.org/10.1016/j.ajic.2004.12.002
- Canova, V., Lederer Schläpfer, H., Piso, R. J., Droll, A., Fenner, L., Hoffmann, T., & Hoffmann, M. (2020). Transmission risk of SARS-CoV-2 to healthcare workers – observational results of a primary care hospital contact tracing. Swiss Medical Weekly, 150(1718).
- World Health Organization. (2020). Rational use of personal protective equipment for coronavirus disease (COVID-19) and considerations during severe shortages.
- Larson, E. L., & Liverman, C. T. (2011). Designing and Engineering Effective PPE. In Preventing Transmission of Pandemic Influenza and Other Viral Respiratory Diseases: Personal Protective Equipment for Healthcare Personnel: Update 2010. National Academies Press (US).
- Mitchell, R., Roth, V., Gravel, D., Astrakianakis, G., Bryce, E., Forgie, S., . . . Vearncombe, M. (2013). Are health care workers protected? An observational study of selection and removal of personal protective equipment in Canadian acute care hospitals. American Journal of Infection Control, 41(3), 240-244. https://doi.org/10.1016/j.ajic.2012.04.332
- Offeddu, V., Yung, C. F., Low, M. S. F., & Tam, C. C. (2017). Effectiveness of Masks and Respirators Against Respiratory Infections in Healthcare Workers: A Systematic Review and Meta-Analysis. Clinical Infectious Diseases, 65(11), 1934-1942. doi:10.1093/cid/cix681
- Jones, R. M., Bleasdale, S. C., Maita, D., & Brosseau, L. M. (2020). A systematic risk-based strategy to select personal protective equipment for infectious diseases. American Journal of Infection Control, 48(1), 46-51. https://doi.org/10.1016/j.ajic.2019.06.023
- Herlihey, T. A., Gelmi, S., Flewwelling, C. J., Hall, T. N. T., Bañez, C., Morita, P. P., . . . Hota, S. (2016). Personal Protective Equipment for Infectious Disease Preparedness: A Human Factors Evaluation. Infection Control & Hospital Epidemiology, 37(9), 1022-1028. doi:10.1017/ice.2016.124
- Verbeek, J. H., Rajamaki, B., Ijaz, S., Sauni, R., Toomey, E., Blackwood, B., . . . Kilinc Balci, F. S. (2020). Personal protective equipment for preventing highly infectious diseases due to exposure to contaminated body fluids in healthcare staff. Cochrane Database of Systematic Reviews(4). doi:10.1002/14651858.CD011621.pub4
- Health and Safety Executive (HSE). (2020). Fit testing face masks to avoid transmission during the coronavirus outbreak.
- Ministry of Health NZ. (2020). COVID-19: Guidelines for the use of personal protective equipment for frontline health care workers.
- New Zealand Government. (2015). Health and Safety at Work Act 2015.
- Worksafe. (2017). Respirator Selection Tool.
- Centers of Disease Control (CDC). (2020). Use of Personal Protective Equipment (PPE) When Caring for Patients with Confirmed or Suspected COVID-19 (PDF, 196 KB).
- Worksafe. (2020). General risk and workplace management.




