About the authors:Christine Barry, BN, BPhEd, GradDipOHS, MPH, is a kaitūhono/connector for My Life My Voice. Christina Severinsen, PhD, is an associate professor in public health in the School of Health Sciences, Massey University, Palmerston North. Andy Towers, PhD, is an associate professor in the School of Health Sciences, Massey University, Palmerston North. This article was accepted for publication in October 2023. |
ABSTRACTAim: This study aims to explore the impact of the Care and Support Worker (Pay Equity) Settlement Act (2017) on the work-related quality of life of homecare support workers. Background: Previous research found negative consequences from the Act’s implementation on care and support workers’ quality of life; however work-related quality of life has not been addressed, providing an opportunity for further investigation. Methodology: The study used a qualitative approach and conducted semi-structured interviews with eight female homecare support workers in 2021. The interviews were analysed thematically using Van Laar et al’s (2007) Work-Related Quality of Life model. Findings: The findings indicate that the Act’s implementation has adversely affected participants’ work-related quality of life. Five key themes were identified, including work re-organisation and intensification, undesirable collegial working relations, and a decline in managerial support and communication. Additionally, pay increments were identified as not keeping up with inflation. Discussion: This study highlights the need for sector-specific guidelines for homecare support workers and standard regulations for providers. The implementation of future legislation should also undergo careful reassessment of how fiscal measures are used. Conclusion: The Care and Support Worker (Pay Equity) Settlement Act (2017) has had a negative impact on participants’ quality of life at work. The findings of this study contribute to the understanding of the unintended consequences of the Act’s implementation on care and support workers and the need for improvements in the sector. |
||||
KEYWORDShomecare, care and support workers, Pay Equity Act 2017, work-related quality of life |
|||||
INTRODUCTION
CARE AND SUPPORT workers play an essential role in health and disability systems worldwide by providing direct care and support in the home, community and disability services (Ravalier et al, 2019; Vassos et al, 2019). They care for older adults and people with various chronic diseases, injuries, disabilities, and mental health and addiction issues (Ministry of Health, 2016; Ravenswood et al, 2015). However research has shown that care and support workers often face poor working conditions and are susceptible to unfavourable pay and marginalisation (Ravalier et al, 2019; Strandell, 2020). Additionally, care and support work is often considered undervalued and gendered as women’s work (Hebson et al, 2015; Stranz & Szebehely, 2018). With the ageing global population, finding ways to support and improve conditions for this vital workforce is important.
Aotearoa New Zealand’s care and support workforce is primarily female, culturally diverse, and ageing, with most workers between 45 and 65 years old (Meagher, 2016; Ravenswood & Douglas, 2017). They mostly work part-time and are not regulated by the Health Practitioners Competence Assurance Act (Ministry of Health, 2016). The demand for care and support services is increasing due to an ageing population and the prevalence of disability and non-communicable diseases (Home and Community Health Association & Lattice Consulting, 2018). However, the working conditions of care and support workers have been affected by class, gendered norms, and hierarchical working relations (Charlesworth & Heap, 2020; Ravenswood & Harris, 2016). Research shows that care work is often undervalued and subjected to gender discrimination (McGregor & Davies, 2019; New Zealand Human Rights Commission, 2012).
Previous research illustrates that financial restructuring of health systems and associated resource constraints have led to intensification of the work of care and support workers, resulting in more significant stress, role ambiguity, reduced staffing rates, and reduced time to complete duties (Strandell, 2020; Trydegård, 2012). Restructuring and resource constraints have further undermined key workplace factors for care and support workers, such as remuneration, employment hours and job security (Stranz & Szebehely, 2018). International research also shows that care and support workers often have low wages, and variable contracts and employment hours, with a high percentage of workers in some countries, such as the United Kingdom, employed under zero-hour contracts (Ravalier et al, 2019; Rubery et al, 2015). In Aotearoa New Zealand, many home and community care workers have limited guaranteed hours of employment and earn the minimum wage (Ravenswood & Douglas, 2017; Ravenswood et al, 2015).
The New Zealand Government enacted the Care and Support Worker (Pay Equity) Settlement Act of 2017 in response to fiscal and work pressures facing care and support workers (Douglas & Ravenswood, 2019; Treasury, 2017). The Act provided $2.048 billion over five years to ensure pay equity for carers in residential, home, community and disability sectors (Care and Support Workers (Pay Equity) Settlement Act, 2017; Ministry of Health, 2018). However, research by Douglas and Ravenswood (2019) found the Act had unintended negative consequences, including reduced hours of work, increased workloads, and heightened work-related stress for care and support workers. Additionally, the home and community care sector saw significant changes in working conditions affecting the job security of Levels 3 and 4 care and support workers, and many were left financially worse off. What was unclear from the Douglas and Ravenswood (2019) investigation was the different ramifications for care and support workers’ wider work life, in particular their work-related quality of life. Recent research by McFadden et al (2021) highlights that support workers’ work-related quality of life is fundamentally associated with their motivation and ongoing contentment at work. The study reported by this article aimed to explore how the Care and Support Worker (Pay Equity) Settlement Act (2017) has affected the work-related quality of life of home and community support workers.
METHOD
Van Laar et al’s (2007) Work-Related Quality of Life model was applied as a framework for a deductive, feminist qualitative investigation into the impact of the Act on support workers’ quality of life. The Work-Related Quality of Life model includes four components: working conditions, stress at work, work-life balance, and career and job satisfaction. This model has been widely used in research and aligns with the deductive approach. The feminist qualitative approach was chosen as the care and support workforce is predominantly female and has a history of gender discrimination.
Participants
The participants in this study were support workers primarily employed in the home and community sector, located in an urban city in the lower North Island of New Zealand. For the purposes of confidentiality, the specific location will remain undisclosed. To recruit participants, a study information sheet was distributed to an industry training organisation (ITO), home and community sector providers, unions, community health and social service organisations, and through word of mouth. Potential participants interested in this study contacted the researcher via phone or email, who checked whether they met the study’s inclusion criteria. The criteria included that participants be English-speaking females, over 18 years of age, currently working as support workers, primarily in a homecare role and holding a Level 3 or 4 experience or qualification. The study’s criteria that participants should be women was to enable women’s voices pertaining to the Act to be heard. Eight participants meeting these criteria were accepted into the study and their identities protected through pseudonyms and participant numbers. The researcher conducted the interviews, which included each participant completing a brief questionnaire enabling the collection of background information (age, years of homecare experience etc), which helped to provide a contextualised understanding of the participants. Table 1 (below) provides key participant demographic information.
Table 1: Key participant demographics
| Participant pseudonym | Age | Level 3 or 4 | Full-time or part-time | Years of experience as support worker |
|---|---|---|---|---|
| Sharon | 65 | 3 | Part-time | 7-10 |
| Lorraine | 47 | 3 | Full-time | 15-18 |
| Jill | 53 | 4 | Full-time | 15-18 |
| Helen | 56 | 3 | Full-time | 7-10 |
| Molly | 66 | 3 | Full-time | 7-10 |
| Cathy | 50 | 3 | Full-time | 11-14 |
| Sarah | not stated | 3 | Full-time | 19+ |
| Tanya | 51 | 4 | Full-time | 11-14 |
Data collection
This study used in-depth, semi-structured, face-to-face interviews for data collection. The interviews were conducted using a set of open-ended questions based on the Work-Related Quality of Life scale. The study received ethical approval from the Massey University Human Ethics Committee, and all participants gave their consent before the interview. The researcher recorded and transcribed the interviews aided by a computerised software transcription service. Identifying information was removed, and the interviews were checked for accuracy by the researcher, and then by participants to ensure data quality.
Data analysis
This study employed Clarke and Braun’s (2014) six-step process of thematic analysis to analyse the data collected from the interviews. Thematic analysis was selected due to the method’s strength in capturing the complexities of meanings and use in exploring experiences from participant interviews (Gavin, 2008; Guest et al, 2012). The transcripts were imported into NVivo software and coded and analysed according to the theoretical concepts of Van Laar et al’s (2007) framework of the four psycho-social subscale components: working conditions, stress at work, work-life balance, and career and job satisfaction. Aspects or concepts within the data perceived as important or significant were systematically assigned to codes under these components, forming coding trees relevant to the research question. Therefore, this study used a combination of deductive and inductive approaches, in which codes emerged from the data and were assigned to the components forming coding trees, and categories were created by addressing similarities and overlaps in codes and coded data. This process involved merging and re-defining codes and resulted in more extensive general codes, with some becoming promoted to potential prominent themes. The first researcher managed the process of code development, and researchers two and three facilitated in the review and refinement of the codes. The four sets of components and their thematic maps were compared to check the possible themes and their relationship to each other. This helped inform the story behind the data and in answering the research question.
RESULTS
The study’s findings on the effects of the Settlement Act on support workers’ work-related quality of life are presented using the four components identified as underlying work-related quality of life: working conditions, stress at work, work-life balance, and job and career satisfaction. These components were used as a framework to analyse and present the data collected from the interviews.
Working conditions
The study found that six support workers reported a significant increase in their pay rate since the Pay Equity Settlement Act was implemented. However half of the participants also reported declining employment hours. This decline was linked to a reduction in guaranteed hours, the hiring of cheaper staff, and less time allocated to clients for care. This suggests that while some workers benefited from the increased pay, they also experienced a reduction in the amount of work available to them. For example:
“Because our pay went up, they probably weren’t quite willing to give us many more hours …”
“They also changed our working … instead of giving an hour to shower, we have to do what we’re doing in three-quarters of an hour, or half an hour. Plus, we were expected to do more in that time, which was less time than what we had then when the pay went up. They didn’t do it so much for existing clients, but they did it for new clients.” (Helen)
“Once pay equity came in … what did they start doing? Us ones that knew what we were doing and had up to Level 3, we weren’t getting the work. They were actually bringing on new ones that they could pay $2 or $3 cheaper.” (Molly)
Some participants also noted that the pay increments they received over the last four years had not kept pace with inflation and living costs, resulting in their wages being similar to the minimum wage. Participants also expressed concerns about the reorganisation and scheduling of their work. Some reported experiencing work intensification, which included pressure to accept extra shifts, working alone in situations meant to be handled by two people, and a lack of time off work. These factors may have negatively affected the overall quality of their working lives.
“You do, at times, feel pressured to fill those [extra] hours, even if you don’t want to. You get the sob story of, ‘But there’s no one else to do the job, and this needs to be done.’ And quite frequently, you do give in when you shouldn’t … Two days off in three weeks is not good.” (Lorraine)
The study also found that the participants perceived a decline in management support and communication following the Act’s implementation. Support was often limited to occasional feedback and emails, with only one provider offering regular staff meetings. This lack of support and communication from management may have added to the stress and dissatisfaction reported by the participants, negatively impacting their overall work-related quality of life.
“After pay equity came in, we didn’t really have much to do with the company itself. For coordinators, it was hard to get through to them. We sat for ages on the phone. There were times when there was an urgent need to get them in, and we got, ‘Just leave a message.’ And so you deal with a problem yourself. And then, later on, you forget to call them back and tell them what happened.” (Sharon)
Participants did not receive adequate management guidance and support, which negatively affected their work. They also mentioned the lack of support forums, which decreased after the Act’s implementation. Participants felt unimportant, unsupported and alone.
For example:
“We don’t have enough contact. We’re out here on our own, and we don’t have office contact …, you just get a text message on the phone. Nobody. They don’t ring.” (Jill)
Changes in how work was organised and reduced communication and support from coordinators led to a decline in the workplace culture in terms of valuing and recognising their roles as support workers. The centralisation of a provider led to the loss of local and regional coordinators and was linked to a lack of concern for support workers, communication problems, and reduced support. Overall, support workers felt that the workplace culture had worsened and that there was less emphasis on their well-being.
Participants felt there was a lack of management support for training, despite the legal requirement under section 12 of the Care and Support Worker (Pay Equity) Settlement Act 2017 that employers must ensure that care and support workers can gain qualifications. They also reported that communication and provision of practical training opportunities were ineffective, often lacking, or absent and worse since the implementation of the Act.
“I think there needs to be ongoing training. They have sent girls in to do catheter bags who have never done a catheter bag in their life. Well, to me, that’s wrong!” (Molly)
“There’s no training … we get taught by each other, not officially by anyone who should be.” (Sharon)
“Well, they say they give us training, but they never do. I’ve never been trained in using a hoist or any equipment ever. Although they will tell you that all girls are trained, they’re not.” (Sarah)
Stress at work
All the study participants experienced intense stress in the workplace due to understaffing, high workload, lack of coordination, and problems with scheduling. They also described feeling pressure to cover extra shifts at the last minute and working for long periods without days off. The participants attributed these issues to the reorganisation of their work following the Act and they reported feeling fatigued and experiencing unsafe working conditions.
“The biggest pressure, again, you get pressured into doing extra hours when you shouldn’t be. You just get too tired.” (Lorraine)
“I [ hurt my hand] … And it was because I was fatigued. I worked too much, slept too little. I did that at work. And it’s fatigue, it’s fatigue. Yeah, such a mess.” (Cathy)
Participants in the study reported stress related to worsening relationships between co-workers due to the reorganisation of work following the Act’s implementation. This behaviour included some co-workers not showing up for shifts and high variability in their availability for shifts, performing care tasks poorly, performing care tasks quickly and leaving client visits as soon as possible, and unpleasant behaviour when communicating with other co-workers. Some of this behaviour resulted in other workers being landed with additional work. These issues compounded and negatively affected client care. One participant reported bullying by co-workers and competition for higher-paying shifts being more prevalent after the Act went into effect.
Work-life balance
Participants reported feeling that their welfare and work-life balance were not considered. This situation had worsened since the Act’s implementation, as a result of work intensification and shortages of available staff. They strongly disagreed that their employers provided adequate facilities and flexibility to accommodate their family life.
“They don’t … Absolutely, they don’t. They don’t talk to you about your needs at all. To be honest with you, they’re just worried about covering these clients.” (Molly)
“We have no coordinator or anybody that gives a toss … so no, it’s non-existent.” (Sarah)
Support workers linked management’s lack of flexibility regarding their employment hours to staff shortages and the centralisation of work.
“Not … so good. Really! No. They are happy if you want an extra shift [laugh], not so happy about time off … I had to do clients before I could go to a funeral because they didn’t have anyone to cover.” (Helen)
“When we had a coordinator, you could ring her, and she would sort it. You know, just cover your shift. It was easy. However, now you don’t do anything because no one will deal with anything. We tend not to now because we know our clients are not going to get covered. So, I think that’s gone by the way, that whole flexibility.” (Sarah)
Five support workers reported that their hours did not suit their circumstances, and the organisation of work significantly affected their ability to achieve work-life balance.
“The split shifts are silly things … I hate the split shift, and I’d like to not do the night shift. But to get enough hours [I’ve] got to. There’s basically no work between one and four, so you’ve got to do the split shifts to get your hours, to get your 40 hours a week.” (Molly)
“No, they don’t suit my personal circumstances. I used to finish work at 4 o’clock. And the hour and a half difference makes a huge difference when your partner goes to bed very early because of his hours. So, with the service review that’s coming up, I’m hoping … I’m hoping to see what changes I can make to bring my finish time down. I don’t mind losing a few hours if I get to spend more time with my family.” (Lorraine)
Support workers felt that management was not considering their wellbeing and were dissatisfied with how management handled shift coverage. These issues indicate a broader workplace culture which prioritises work over personal life and shows little willingness to make changes.
Career and job satisfaction
The implementation of the Act has negatively impacted the job satisfaction of the support workers due to poor work organisation and communication. Additionally, the workers reported not receiving recognition or appreciation from management and feeling undervalued and disrespected. These issues can have a negative impact on employee morale and may contribute to high turnover.
“No appreciation whatsoever. You would ring, and they didn’t want to know what your name was – they want to know what your number was.” (Molly)
“Being paid on the higher rate doesn’t mean they value me! It just means I’m paid on the higher rate. And that’s all there is to it.” (Jill)
The participants’ responses indicate that management does not seem to understand or appreciate fully the importance of their role and that they are not taking the views and feedback of the support workers regarding client care seriously. This lack of consideration and sincerity can lead to a lack of trust and engagement among support workers, which can negatively impact the quality of client care.
“I sent [so many] complaints to that person in the office, … but they don’t answer [my many] complaints. And in the end, I got told, ‘Oh, sorry, they went to my junk file.’ I mean, now … that’s our leadership! They are all legit ones, clients missing care, you know.” (Sarah)
The participants’ responses clearly indicated they felt undervalued and unappreciated in their roles. They felt their contributions were not recognised, and management did not value their work. This lack of recognition can lead to a lack of job satisfaction, which can negatively affect the quality of life at work and the workers’ perceptions of pay equity.
“And even now, the pay is terrible. We [are] only $1 more than the living wage. So, it’s a bit of a joke now! It was great to start with because we’re to go from $14 to $21 [which] was pretty cool. And then we’ve just had 50c increments each year; we just went up to $25. I’ve just gone up to $25.” (Molly)
Deductive thematic analysis identified five key themes in the provided information: organisation and intensity of work; stress related to organisation and intensity of work; organisation and intensity of work and work-life balance; co-worker working relations; and management support and communication affecting job satisfaction. These themes highlight the negative impact of the Care and Support Worker (Pay Equity) Settlement Act (2017) on the work-related quality of life for these homecare support workers. The themes are illustrated in a flow diagram (Figure 1, below) which shows how the implementation of the Act has led to these adverse effects.
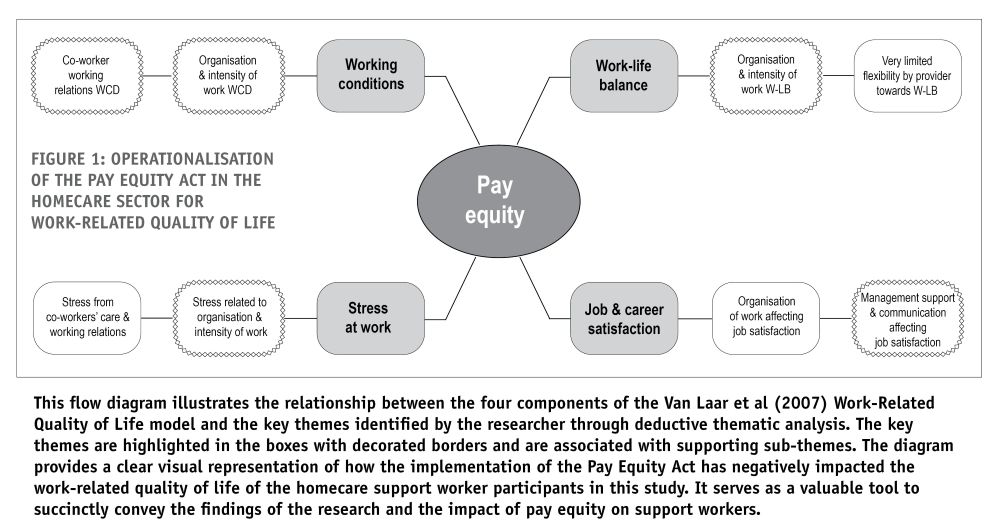
DISCUSSION
This study was conducted to investigate the effects of the Pay Equity Settlement Act 2017 on support workers’ work-related quality of life in Aotearoa New Zealand. The research builds on previous work by Douglas and Ravenswood (2019) on the unintended consequences of the Act’s implementation on the quality of life of care and support workers. The study used the Van Laar et al (2007) Work-related Quality of Life model to identify five key themes related to working conditions, stress at work, work-life balance, and job satisfaction. This researcher’s study found that the Act negatively impacted the work-related quality of life of these home and community support worker participants.
A significant finding of the study was the negative impact of the re-organisation and intensification of work on the participants’ work-related quality of life. The employers’ response to the Act caused changes in work schedules, workloads, and work expectations that offset the initial benefits of the increased pay rates. Participants had less time to perform tasks and felt rushed and pressured to complete them, which decreased the time allocated for client care. These findings were consistent with previous research from Nordic countries and Douglas and Ravenswood (2019). It is also important to note that although support workers’ rates of pay were increased under this Act, nurses in this sector did not receive corresponding pay increases (Douglas & Ravenswood, 2019).
The findings of this study point to the need for more regulation of homecare services, including guidelines relating to time frames for the provision of care and nationally applied practice guidelines specific to support workers in the homecare sector. The study highlights the importance of effective communication and management support in the homecare industry to improve job satisfaction, training and the quality of care provided to clients. Additionally, it emphasises the need for more oversight in the homecare industry to ensure the safety and wellbeing of both support workers and clients. This oversight could also extend to nurses working in the homecare sector.
The findings of this study suggest the Act has negatively affected the work-related quality of life of homecare support workers employed in an urban lower North Island area of Aotearoa New Zealand. The re-organisation and intensification of work, lack of management support, and poor collegial working relations all contributed to a negative impact on the work-related quality of life of these workers. The findings of this study highlight the need for further examination of the effects of work intensification, standard regulations for homecare providers, and development of nationally applied sector-specific practice guidelines for support workers in the homecare sector. Finally, the study illustrates the need for more research into the effects of the Act on the homecare sector and the welfare of support workers and clients. There are implications for safe practice, including heightened potential for errors and accidents affecting client and support worker safety. Such negative circumstances impinge on the provision of care and affect the fundamental purpose of care and support work.
LIMITATIONS
The study has limitations, including a small sample size, and the potential for information provided to be affected by selective memory bias and telescoping. This researcher addressed four of Van Laar et al’s (2007) six psycho-social scales to enable an appropriate scope and research time frame for this study.
CONCLUSION
This study found the implementation of the Care and Support Worker (Pay Equity) Settlement Act (2017) had a significant, negative impact on the work-related life of the participants. It found that the re-organisation and increased intensity of work, along with a decline in managerial support, had negatively affected the participants’ working conditions and job satisfaction. The study supports earlier findings of unintended consequences of the Act’s implementation. This study highlights the need for more regulation of service providers to address the shrinking time frames for providing care to clients, and the development of specific homecare support worker guidelines, to improve the work conditions and quality of life of homecare support workers.
REFERENCES
Care and Support Workers (Pay Equity) Settlement Act 2017.
Charlesworth, S., & Heap, L. (2020). Redressing gendered undervaluation in New Zealand aged care: Institutions, activism and coalitions. Journal of Industrial Relations, 62(4), 608-629.
Clarke, V., & Braun, V. (2014). Thematic analysis. In T. Teo (Ed.), Enyclopedia of Critical Psychology (pp. 1947-1952). Springer New York.
Douglas, J., & Ravenswood, K. (2019). The value of care: Understanding the impact of the 2017 Pay Equity Settlement on the residential aged care, home and community care and disability support sectors. New Zealand Work Research Institute.
Gavin, H. (2008). Designing qualitative research. Sage Publications.
Guest, G., MacQueen, K., M, & Namey, E., E. (2012). Applied thematic analysis. Sage Publications.
Hebson, G., Rubery, J., & Grimshaw, D. (2015). Rethinking job satisfaction in care work: Looking beyond the care debates. Work, Employment and Society, 29(2), 314-330.
Home and Community Health Association & Lattice Consulting. (2018). Spreading our wings.
McFadden, P., Ross, J., Moriarty, J., Mallett, J., Schroder, H., Ravalier, J., Manthorpe, J., Currie, D., Harron, J., & Gillen, P. (2021). The role of coping in the wellbeing and work-related quality of life of UK health and social care workers during COVID-19. International Journal of Environmental Research and Public Health, 18(2), 815.
McGregor, J., & Davies, S. G. (2019). Achieving pay equity: Strategic mobilization for substantive equality in Aotearoa New Zealand. Gender, Work & Organization, 26(5), 619-632.
Meagher, G. (2016). Valuing care work and care workers: Workforce and equal pay issues in New Zealand aged residential care. Macquarie University.
Ministry of Health. (2016). Health of the Health Workforce 2015.
Ministry of Health. (2018). Summary of the pay equity for care and support workers: Overview and timeline.
New Zealand Human Rights Commission. (2012). Caring counts –Tauitiaki tika.
Ravalier, J., Morton, R., Russell, L., & Rei Fidalgo, A. (2019). Zero‐hour contracts and stress in UK domiciliary care workers. Health & Social Care in the Community, 27(2), 348-355.
Ravenswood, K., & Douglas, J. (2017). The New Zealand Aged Care Workforce Survey 2016. New Zealand Work Research Institute.
Ravenswood, K., Douglas, J., & Teo, S. (2015). The New Zealand Aged Care Workforce Survey 2014.
Ravenswood, K., & Harris, C. (2016). Doing gender, paying low: Gender, class and work-life balance in aged care. Gender, Work & Organization, 23(6), 614-628.
Rubery, J., Grimshaw, D., Hebson, G., & Ugarte, S. M. (2015). ‘It’s all about time’: Time as contested terrain in the management and experience of Domiciliary Care Work in England. Human Resource Management, 54(5), 753-772.
Strandell, R. (2020). Care workers under pressure – A comparison of the work situation in Swedish home care 2005 and 2015. Health & Social Care in the Community, 28(1), 137-147.
Stranz, A., & Szebehely, M. (2018). Organizational trends impacting on everyday realities: the case of Swedish eldercare. In K. Christensen & D. Pilling (Eds.), The Routledge Handbook of Social Care Work Around the World (pp. 45-57).
Treasury. (2017, July 28). Budget 2017 Information Release. New Zealand Government.
Trydegård, G.-B. (2012). Care work in changing welfare states: Nordic care workers’ experiences. European Journal of Ageing, 9(2), 119.
Vassos, M., Nankervis, K., Skerry, T., & Lante, K. (2019). Can the job demand-control-(support) model predict disability support worker burnout and work engagement? Journal of Intellectual & Developmental Disability, 44(2), 139-149.
Van Laar, D., Edwards, J. A., & Easton, S. (2007). The Work-Related Quality of Life scale for healthcare workers. Journal of Advanced Nursing, 60(3), 325-333.


 Christine Barry
Christine Barry Christina Severinson
Christina Severinson Andy Towers
Andy Towers Ten new forensic inpatient beds have been made available at the Regional Forensic Psychiatric Service at Waikato Hospital to expand forensic mental health capacity for adults in prison or on remand in Health New Zealand’s Midland region.
Ten new forensic inpatient beds have been made available at the Regional Forensic Psychiatric Service at Waikato Hospital to expand forensic mental health capacity for adults in prison or on remand in Health New Zealand’s Midland region.

 A passion for his Māori culture and a desire to make AI accessible to everyone inspired Troy Baker, Senior ICT Specialist, Health New Zealand to develop BroPilot – a culturally grounded way of working with Microsoft Copilot that reflects Māori values, whakaaro, and real lived experience.
A passion for his Māori culture and a desire to make AI accessible to everyone inspired Troy Baker, Senior ICT Specialist, Health New Zealand to develop BroPilot – a culturally grounded way of working with Microsoft Copilot that reflects Māori values, whakaaro, and real lived experience.


